Breast reconstruction is a surgical procedure that rebuilds the shape of the breast after a mastectomy. For many women, it helps restore body image, confidence, and a sense of wholeness after breast cancer treatment. There is no one-size-fits-all approach. Your best option depends on your health, cancer treatment plan, body type, and personal goals.
When can Breast Reconstruction Be Done?
1] Immediate Reconstruction
Performed at the same time as your mastectomy – fewer surgeries overall
You wake up with a breast shape already in place
2] Delayed Reconstruction
Done months or years after mastectomy
May be recommended if you need radiation therapy, allows more time to consider options
Both approaches are safe and common. Your surgical team will help guide the timing.
Main Types of Breast Reconstructions
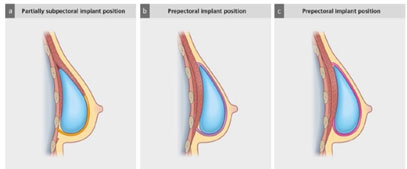
- Implant-Based Reconstruction
This method uses a silicone breast implant to create breast shape.
How it Works:
A temporary tissue expander may be placed first to stretch the skin
Later replaced with a permanent implant
Pros:
Shorter surgery
No Additional scars on other body areas & faster recovery
Considerations:
Implants may need replacement in the future & may have slightly higher risk of complications after radiation
- Flap ( Autologous) Reconstruction
This technique uses your own tissue (skin, fat, sometimes muscle) from another area of your body.
Common donor areas:
- Abdomen ( DIEP or TRAM flap )
- Back ( Latissimus dorsi flap)
- Thigh or buttocks (less common)
Pros:
- More natural look and feel
- Long- lasting results
Considerations:
- Long surgery and recovery
- Scar at donor site
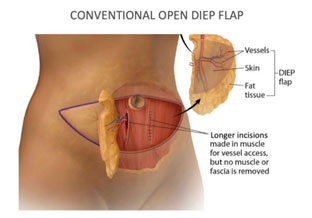
What is DIEP Flap surgery?
DIEP ( Deep Inferior Epigastric artery Perforator)flap uses skin and fat from the lower abdomen without removing abdominal muscle .
Benefits :
Natural breast shape
“Tummy tuck” effect
Lower risk of abdominal weakness compared to older techniques
Not everyone is a candidate –your surgeon will evaluate blood supply and body tissue availability.
Nipple and Areola Reconstruction
This is usually the final stage of reconstruction.
Options include :
- Surgical nipple reconstruction
- 3D nipple tattooing
- Medical tattooing for color matching
- Some patients choose to skip this step –it’s completely personal.
What is Recovery Like?
Recovery depends on the type of reconstruction:
Implant reconstruction:
- 2 – 4 weeks initial recovery
- Return to light activities within 2 – 3 weeks
Flap reconstruction:
- 4 – 8 weeks recovery
- Longer hospital stay
Common temporary Symptoms:
- Swelling
- Tightness
- Fatigue
- Mild to moderate discomfort
Risk and Complications
- Infection
- Bleeding
- Delayed wound healing
- Implant rupture ( implant cases)
- Flap failure (rare in experienced centers )
Choosing a qualified plastic surgeon significantly reduces risks.
Emotional Considerations
Reconstruction is not just physical – it’s emotional.
Many patients report:
- Improved body confidence
- Better clothing fit
- Increased sense of closure
However, it’s also normal to experience mixed emotions. Support groups and Counselors can help.
How to Decide What’s Right for you
Ask yourself:
- Do I want the most natural feel possible?
- Am I comfortable with implants?
- Do I want the shortest recovery?
- Will I need radiation therapy?
- How many surgeries am I comfortable having?
Conclusion
Breast reconstruction after mastectomy offers many options to help restore the shape of the breast and support a woman’s sense of well being after breast cancer treatment. Each approach – whether implant based or using your own tissue – has its own advantages, recovery process and considerations. Breast reconstruction after mastectomy is a highly personal decision- and there is no right or wrong choice.
With careful planning and guidance from experienced healthcare professionals, breast reconstruction can be an important step in the healing process- helping many women regain confidence, comfort and a positive sense of body image as they move forward in treatment. The goal is not just rebuilding a breast – it’s supporting your healing journey.
Dr. Nitu Joy
MBBS, M.S ( General Surgery ), MCh ( Plastic and Reconstructive surgery)
Consultant – Plastic and Reconstructive Surgeon















