Yesterday, April 19th, marked World Irritable Bowel Syndrome (IBS) Day. Patients with IBS often feel frustrated, unheard, or even embarrassed by their digestive systems. If you’ve ever felt like your gut has a mind of its own – and that mind is currently throwing a tantrum – you are certainly not alone.
IBS is one of the most common gastrointestinal disorders worldwide, affecting roughly 10-15% of the population. The good news is that, while it can be a literal pain in the gut, it is highly manageable. Let’s break down what is happening inside and how we can get you back to feeling like yourself.
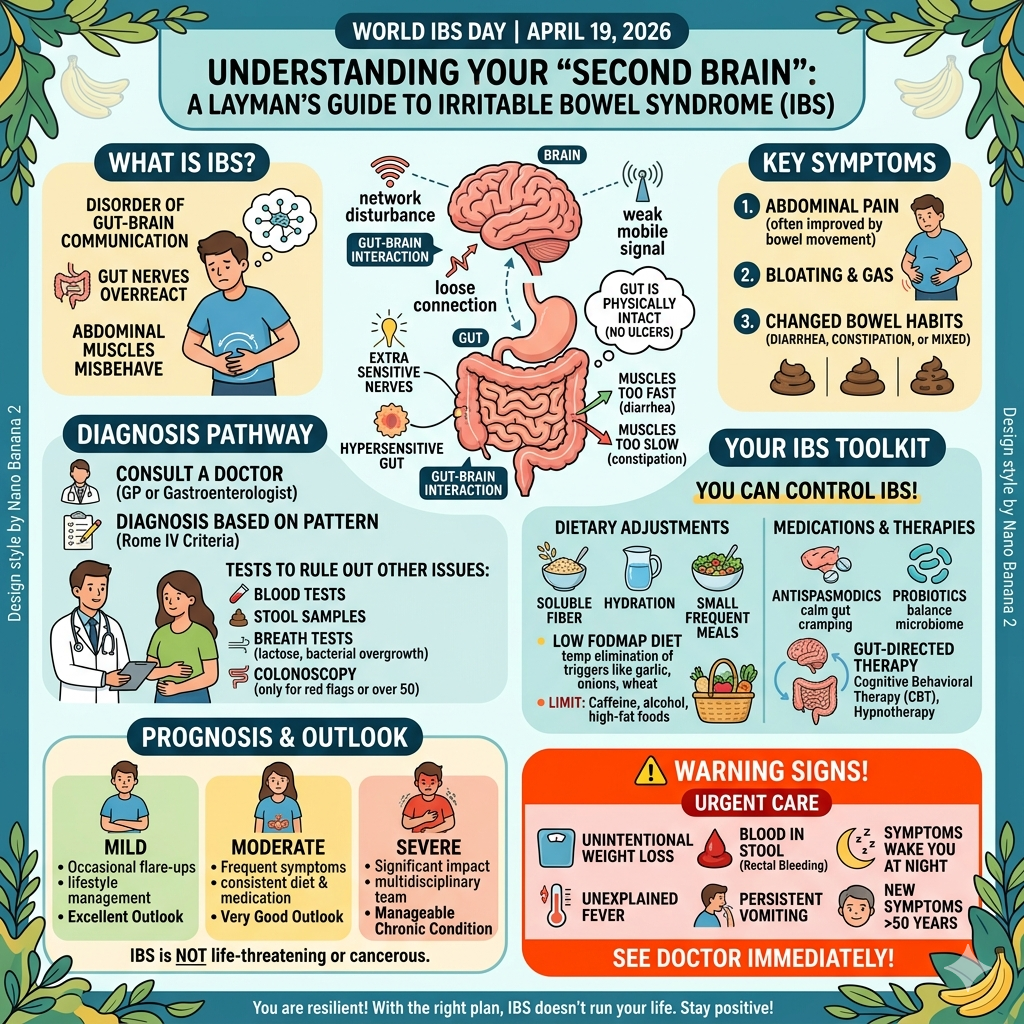
What Exactly is IBS?
Think of your brain and your gut (stomach and intestines) like two people talking on a mobile phone. In a healthy person, the network is perfect and the voice is clear. But in IBS, there is a lot of “network disturbance” or static on the line.
Even though the phone (your digestive system) is not broken and has no physical damage like wounds or ulcers, it just doesn’t work properly because the signal is weak or confusing. We call this a “loose connection” between the brain and the gut. Because of this:
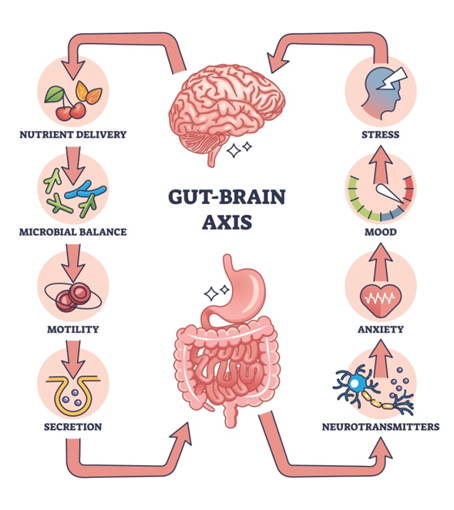
- The Gut is Extra Sensitive: Even a little bit of normal gas or digestion feels like a lot of pain.
- Wrong Speed: The muscles in your stomach might work too fast (causing diarrhea) or too slow (causing constipation).
- Mistaken Signals: Your brain overreacts to things that shouldn’t normally cause trouble.
In short, your body is physically “All Correct,” but the way it “talks” to your brain is out of balance.
When to Suspect You Have It
IBS typically presents as a combination of three main symptoms:
- Abdominal Pain: Usually related to bowel movements (it might feel better or worse after you go).
- Bloating: That “inflated balloon” feeling in your abdomen.
- Changed Bowel Habits: This could be diarrhea (IBS-D), constipation (IBS-C), or a mix of both (IBS-M).
The Path to Diagnosis: What to Expect
If you suspect you have IBS, your first stop should be your Primary Care Physician or a Gastroenterologist. We don’t have a single “IBS blood test.” Instead, we use a set of clinical guidelines called the Rome IV Criteria to identify patterns in your symptoms.
Common tests to rule out “mimics” (like Celiac disease or IBD) include:
- Blood Tests: To check for inflammation markers or anemia.
- Stool Samples: To look for infections or hidden inflammation.
- Breath Tests: To check for lactose intolerance or Small Intestinal Bacterial Overgrowth (SIBO).
- Colonoscopy: Generally only recommended if you have “red flag” symptoms or are over the age of 45-50.
Taking Control: Treatment and Lifestyle
Managing IBS is rarely about a single “magic pill.” It’s about a toolkit.
1. Dietary Adjustments
What you eat matters, but it isn’t the cause of IBS—it’s a trigger.
- What to embrace: Soluble fiber (like oats), hydration, and smaller, frequent meals.
- The Low FODMAP Diet: This is a temporary elimination diet that limits specific fermentable carbohydrates (like garlic, onions, and wheat) that gas-producing bacteria love.
- What to limit: Caffeine, alcohol, high-fat processed foods, and excessive artificial sweeteners (sorbitol/mannitol).
2. Medications & Therapies
- Antispasmodics: To calm gut cramping.
- Probiotics: Specific strains can help balance your microbiome.
- Gut-Directed Therapy: Techniques like Cognitive Behavioral Therapy (CBT) or hypnotherapy are incredibly effective at “silencing” the overactive gut-brain signal.
Prognosis: What Does the Future Look Like?
IBS is a chronic condition, but it is not life-threatening, and it does not lead to cancer or inflammatory bowel disease (IBD).
| Severity | Typical Experience | Long-term Outlook |
| Mild | Occasional flare-ups triggered by specific foods or stress. | Excellent. Usually managed with minor lifestyle tweaks. |
| Moderate | Frequent symptoms that may interfere with work or social life. | Very Good. Requires a consistent diet and perhaps daily medication. |
| Severe | Constant symptoms that significantly impact quality of life. | Manageable. Requires a multidisciplinary team (Doc + Dietitian + Psychologist). |
When to Seek Urgent Attention
While IBS is uncomfortable, it shouldn’t be “scary.” If you experience any of the following Red Flags, please see a doctor immediately, as these are not typical of IBS:
- Unintentional weight loss.
- Blood in your stool (rectal bleeding).
- Symptoms that wake you up from a sound sleep at night.
- Unexplained fever or persistent vomiting.
- New symptoms starting after the age of 50.
Final Thought:
Your gut might be sensitive, but you are resilient. With the right plan, IBS doesn’t have to run your life. Happy (belated) World IBS Day – here’s to a calmer digestive journey ahead!
Dr. Somnath Chatterjee MD (Anaes), FRCA, EDIC, FFICM
Medical Director
Prakriya Hospitals, Bengaluru