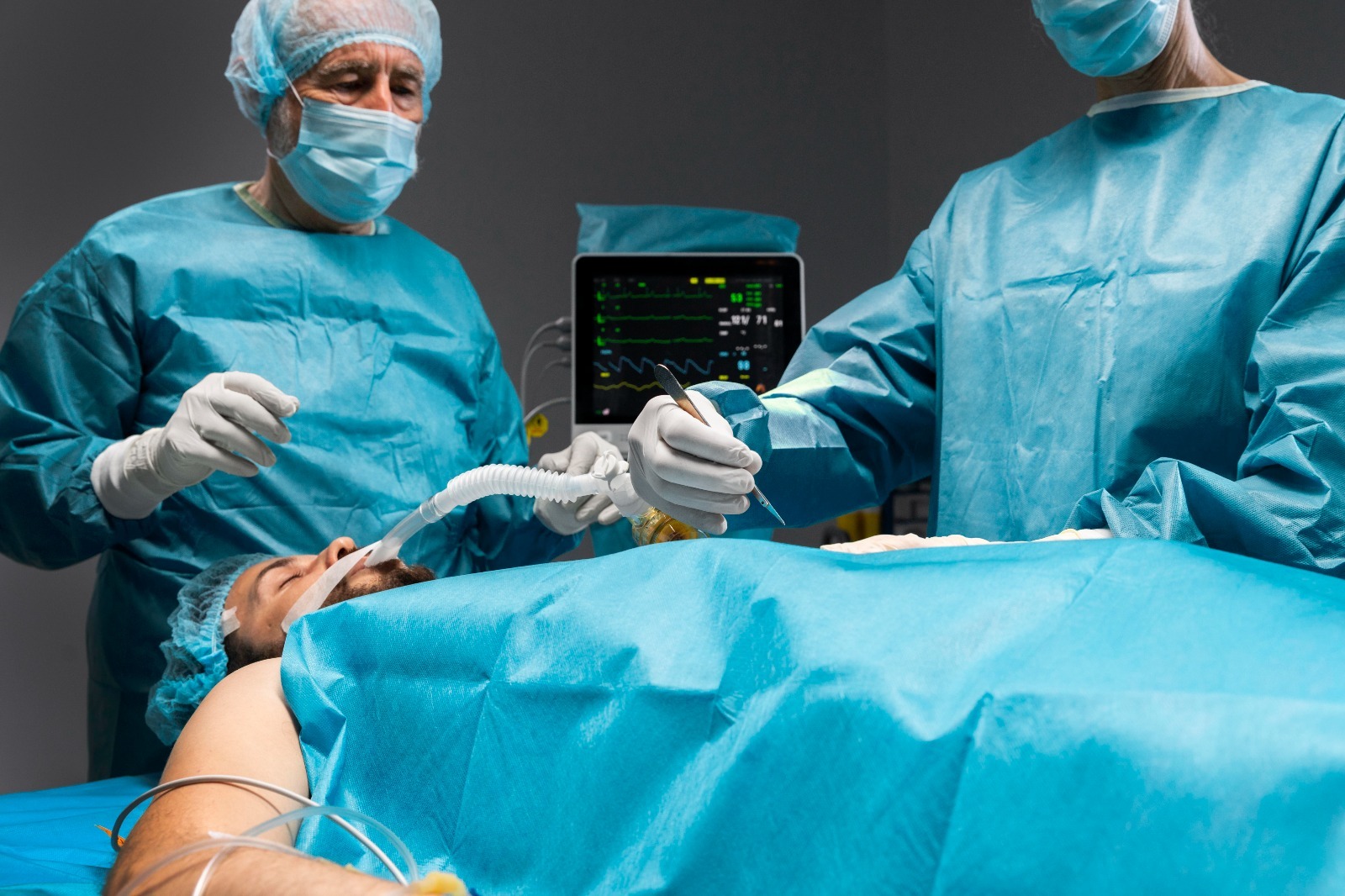
In the emergency room, few situations demand faster decision-making than an unstable patient with abdominal pain. Hypotension, poor perfusion, and concerning imaging almost reflexively push clinicians toward one conclusion – a surgical abdomen.
But every once in a while, medicine reminds us to pause.
A 31-year-old male arrived in the emergency department with a history of diffuse abdominal pain for two months, which had worsened recently. He also reported a couple of episodes of loose stools and a persistent productive cough over the same duration.
At presentation, he was critically ill.
His blood pressure was 80/60 mmHg, and he showed clear signs of poor peripheral perfusion. Surprisingly, his pulse was only 92 beats per minute, and oxygen saturation remained normal on room air. Initial labs revealed a striking finding – severe anemia with hemoglobin around 5 g/dL.
This was no longer just abdominal pain. This was shock with a suspected intra-abdominal cause.
Given the clinical picture, the immediate concern was a surgical abdomen, possibly due to a hollow viscus perforation. Imaging appeared to support this assumption.
A contrast-enhanced CT scan of the abdomen revealed multiple thick-walled, peripherally enhancing collections in the lower abdomen and pelvis. There were pockets of free air within these collections, raising strong suspicion for a sealed perforation. In addition, there was omental thickening, nodularity, and clumping of bowel loops-features that further strengthened the impression of an intra-abdominal surgical pathology.
At this point, the case seemed straightforward.
And yet, something didn’t quite fit.
Despite alarming imaging findings, the clinical course told a different story. The symptoms had been ongoing for two months—unusual for an acute surgical catastrophe. There were no clear signs of diffuse peritonitis. And importantly, the patient had a persistent cough that could not be ignored.
This mismatch between acute radiological findings and a chronic clinical history prompted a broader evaluation.
A CT scan of the chest provided the turning point.
It revealed bilateral areas of consolidation with cavitary changes, along with mediastinal lymphadenopathy showing calcification. These findings raised suspicion for an infectious etiology.
To confirm this, bronchoscopy was performed, and bronchoalveolar lavage tested positive for acid-fast bacilli.
The diagnosis was now clear.
This was not a primary surgical abdomen. This was disseminated tuberculosis with significant abdominal involvement, mimicking a surgical emergency.
The abdominal findings were explained in a new light. Tuberculosis had led to peritoneal inflammation, loculated collections, and even features suggestive of early cocoon formation. The presence of free air, initially alarming, likely represented a sealed perforation rather than an active surgical emergency.
Management shifted accordingly.
The patient was aggressively resuscitated with intravenous fluids and required packed red blood cell transfusions for severe anemia. He was closely monitored in the ICU and started on supportive care along with empirical antibiotics initially. With stabilization and confirmation of diagnosis, the focus moved toward appropriate anti-tubercular management.
Over time, the patient improved clinically and was eventually discharged in a stable condition – without undergoing surgery.
This case underscores an important clinical lesson.
Not every patient who presents with shock and imaging suggestive of perforation requires immediate surgical intervention. In regions where tuberculosis is prevalent, abdominal TB remains a great mimicker, capable of presenting as abscess, obstruction, peritonitis, or even perforation.
What made the difference here was the willingness to question the initial assumption. The chronicity of symptoms, the associated respiratory complaints, and the absence of overt peritonitis created just enough doubt to look deeper.
Dr. Monika Safaya
MBBS, MEM, MRCEM
Consultant – Emergency Medicine